NIST study shows alarming changes in the illegal drug supply.
An animal tranquilizer has flooded the illicit drug market in Maryland, according to a new study by the National Institute of Standards and Technology (NIST) and the Maryland Department of Health. When injected, the tranquilizer, xylazine, causes wounds at the injection site, in some cases so severe that people need to have their arms or legs amputated.
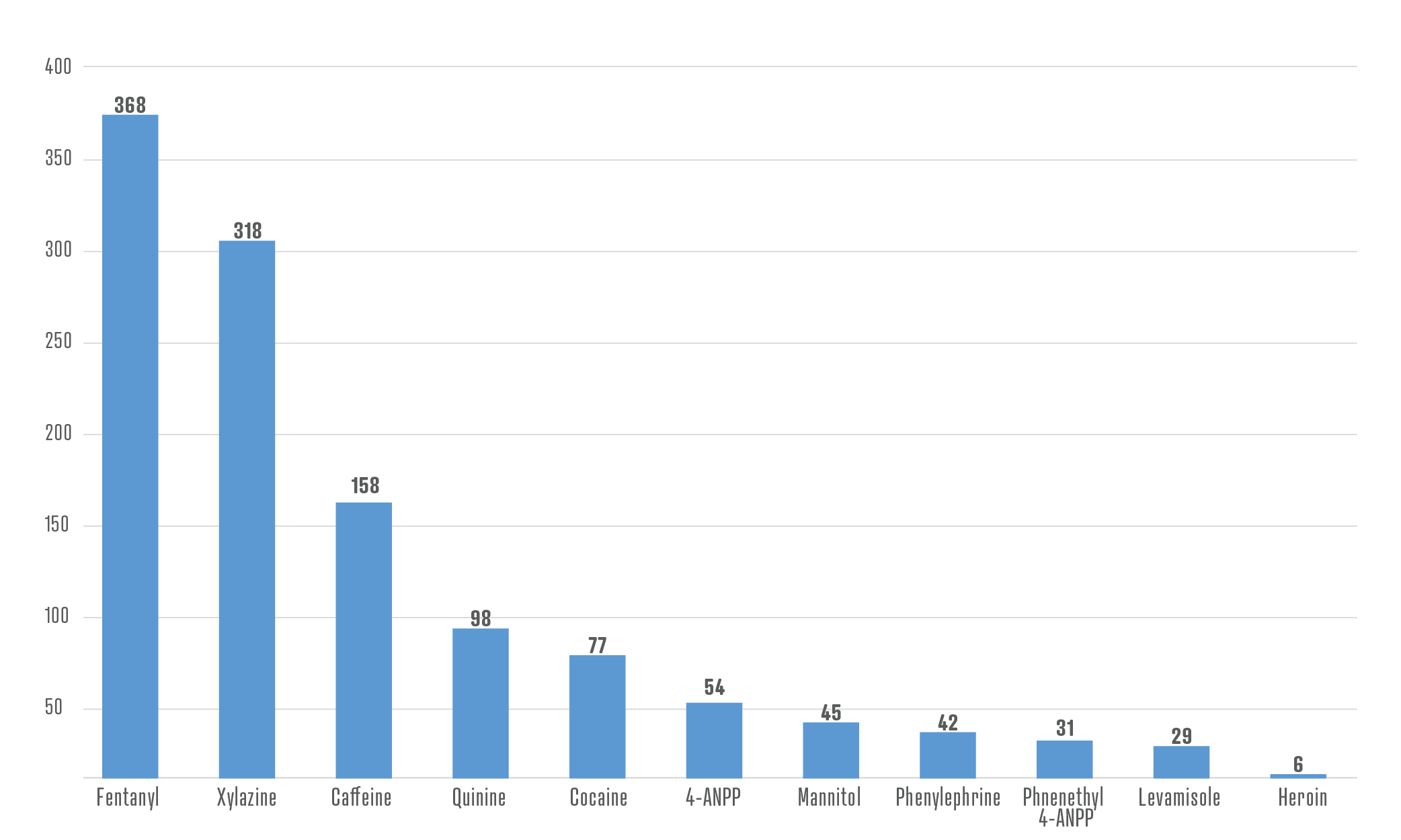
The study, which analyzed residues from illegally purchased drugs to determine the chemical compounds the drugs contained, found xylazine in 80% of samples that included the synthetic opioid fentanyl. The residue samples were collected from empty bags and paraphernalia voluntarily provided by people who used illegal drugs in Maryland during the 11-month period from October 2021 through August 2022.
“We knew xylazine was present in the drug supply,” said Meghan Appley, a research scientist working at NIST and an author of the study. “But we did not expect the prevalence to be nearly so high.”
The study, conducted as part of NIST’s Rapid Drug Analysis and Research, or RaDAR program, was published in the journal Forensic Chemistry.
Another alarming result from the study is that fentanyl, a synthetic opioid that mimics the effects of heroin but is far more potent, has almost completely displaced heroin in Maryland’s underground drug market. Of the 496 samples tested in the study, only six, or 1.2%, contained heroin.
“If you think you’re buying heroin,” said Ed Sisco, the NIST research chemist who led the study, “you’re not.”

Although the drug samples tested in this study all came from Maryland, the results may be a harbinger for other states.
Fentanyl is driving the overdose epidemic that in 2021 took the lives of more than 107,000 people in the U.S. Synthetic opioids like fentanyl are so deadly in part because underground chemists constantly cook up new variants of them, called analogues, some of which are extraordinarily potent. People often don’t know which drugs they are taking, which increases the risk of overdose.
The residue samples analyzed in this study were collected by wound care nurses and other designated staff members at needle exchange centers funded by the Maryland Department of Health. The staff members collected the residue samples by running cotton swabs over empty bags or paraphernalia provided by people who use drugs, then they sent the swabs to NIST for analysis.
At NIST, Sisco and Appley analyzed the samples using a technique that can detect multiple types of drugs present in the sample. The technique, called direct analysis in real time mass spectrometry, or DART-MS, is sensitive enough to pick up small amounts of fentanyl analogues or other drug variants, even when mixed with much larger amounts of regular fentanyl. Conventional lab methods often miss these small but potentially deadly components of a drug mixture.
Read Ed Sisco’s blog post about his work helping communities monitor changes in their illegal drug supply.
The results from the analysis are shared at the needle exchange centers so that people know what compounds are present in the drugs they are buying. This information sharing strategy is meant to reduce the harm caused by drug addiction. The idea is that when people get reliable information, they can modify their behavior to reduce the risks. For instance, they might make sure not to use alone and to have the opioid antidote naloxone handy so that someone is there to save them if they overdose.
NIST also shares the results more broadly with public health authorities, to provide an early warning when new drugs or highly potent drug analogues hit the streets.
“With this program, we can detect new substances more quickly than before,” said study co-author Erin Russell, who leads the Maryland Department of Health’s Center for Harm Reduction Services. “And we can mobilize resources where they’re needed based on what we’re seeing in the data.”
Although this study only includes data from samples collected through August of last year, the RaDAR program continues. In more recent months, another veterinary sedative, medetomidine, has started turning up in the samples, highlighting the ongoing risks from an ever-changing drug supply.
Paper: M. Appley, E. Robinson, A. Thomson, E. Russel, E. Sisco. An Analytical Platform for Near Real-Time Drug Landscape Monitoring using Paraphernalia Residues. Forensic Chemistry. Published online March 16, 2023. DOI: 10.1016/j.forc.2023.100489
Source: NIST.gov

